
Are We Traumatized or Something Else? Rethinking How We Talk About Trauma
Understanding Trauma, PTSD, and Why Language Matters

Many of us have casually said things like, “I’m traumatized” or “I have PTSD from that.” These phrases have become part of everyday speech, especially online. But trauma and PTSD have specific meanings, and understanding them can help us speak about our experiences—and others’ experiences—with more care, accuracy, and compassion. Recognizing that not all emotional pain is trauma does not diminish the seriousness of traumatic experiences. Rather, it helps us describe different forms of suffering more accurately.
This article explores what trauma actually refers to, why self‑diagnosis can be complicated, and how using more nuanced language can support deeper healing.
What Is Trauma in Psychology?
In clinical psychology, trauma usually refers to experiences that overwhelm a person’s ability to cope and create lasting emotional or physiological distress. These experiences often involve threat, harm, or profound helplessness. At the same time, many painful life experiences do not meet the clinical definition of trauma, even though they can still be deeply meaningful and difficult.
What Trauma Really Means
Trauma is not the event itself—it’s the body’s response to an overwhelming or threatening experience. For example, if you fall off a bike and break your arm, the trauma isn’t the fall; it’s the injury. Similarly, in mental health, trauma refers to the physiological and emotional impact of an event, not the event alone.
Different people can have very different responses to the same experience. What overwhelms one person’s nervous system may not overwhelm another’s. Trauma is about the body’s reaction, not about the “severity” of the event.
How the Body Responds to Trauma
Some researchers, including Bessel van der Kolk, describe how trauma may influence the brain and nervous system long after the event. He suggests that reminders of danger can activate stress responses, leading to strong emotions, physical sensations, or protective behaviours. These reactions can feel confusing or distressing, especially when they show up unexpectedly.
Not everyone responds to trauma in the same way, and not all overwhelming experiences lead to long‑term symptoms. But for some people, trauma can shape how the body interprets safety, threat, and connection.
Big T Trauma and Little T Trauma

These terms are sometimes used to describe different types of overwhelming experiences:
- Big T Trauma refers to events that are clearly threatening or catastrophic, such as natural disasters, assaults, or serious accidents. These experiences can create intense distress and may overwhelm a person’s ability to cope. Emotional suffering rarely comes from a single source. Emotional suffering rarely comes from a single source. Psychological distress is often shaped by a mix of biological, psychological, and social factors.
- Little T Trauma refers to ongoing or repeated stressors that may not be life‑threatening but can still affect emotional wellbeing over time. Examples include chronic conflict, bullying, financial instability, or major life transitions.
These categories are descriptive, not diagnostic. People’s responses vary widely, and both types of experiences can be meaningful and impactful.
The Window of Tolerance: Finding Your “Optimal Zone”
If trauma is the body’s response to being overwhelmed, the Window of Tolerance (a term coined by Dr. Dan Siegel) is the map that helps us understand our capacity to handle that overwhelm.
Think of your nervous system like a hallway. When you are inside your "Window," you are in the Optimal Zone. You might feel stressed, sad, or angry, but you are still "online." You can think clearly, communicate your needs, and process your emotions without being hijacked by them.
However, when an experience—like a "Big T" event or a cumulative "Little T" stressor—pushes us out of this window, our body flips into survival mode:
1. Hyper-arousal (The "Too Much" Zone)
This is the Fight or Flight response. When you are pushed out the top of your window, your nervous system is stuck on "high."
- How it feels: Racing heart, obsessive thoughts, panic, anger, or feeling "jittery" and hyper-vigilant.
- The impact: It’s hard to rest or feel safe because your body is convinced a threat is imminent.
2. Hypo-arousal (The "Too Little" Zone)
This is the Freeze response. When you are pushed out the bottom of your window, your nervous system "shuts down" to protect you from further pain.
- How it feels: Numbness, exhaustion, brain fog, feeling "spaced out" (dissociation), or a sense of hopelessness.
- The impact: It can feel like you are moving through molasses or watching your life happen from a distance.
Why Precise Language Helps You Stay in the Window
The goal of therapy isn't just to "fix" the trauma, but to help you widen your window. When we use casual labels like "I'm so triggered," we sometimes accidentally push ourselves further into hyper-arousal by amping up the threat level in our minds.
By using the nuanced language we discussed earlier—saying, "I feel a lot of tension in my chest right now because I'm overwhelmed"—you are practicing self-regulation. You are naming the experience from inside the window, which helps your nervous system stay grounded and prevents a full-blown survival response.
Why Self‑Diagnosis Can Be Complicated
It’s understandable to want language that helps us feel seen or connected. Social media often normalizes using clinical terms casually, and many posts about trauma or PTSD can feel relatable. But self‑diagnosis can be misleading for several reasons:
Misinformation and Overlap
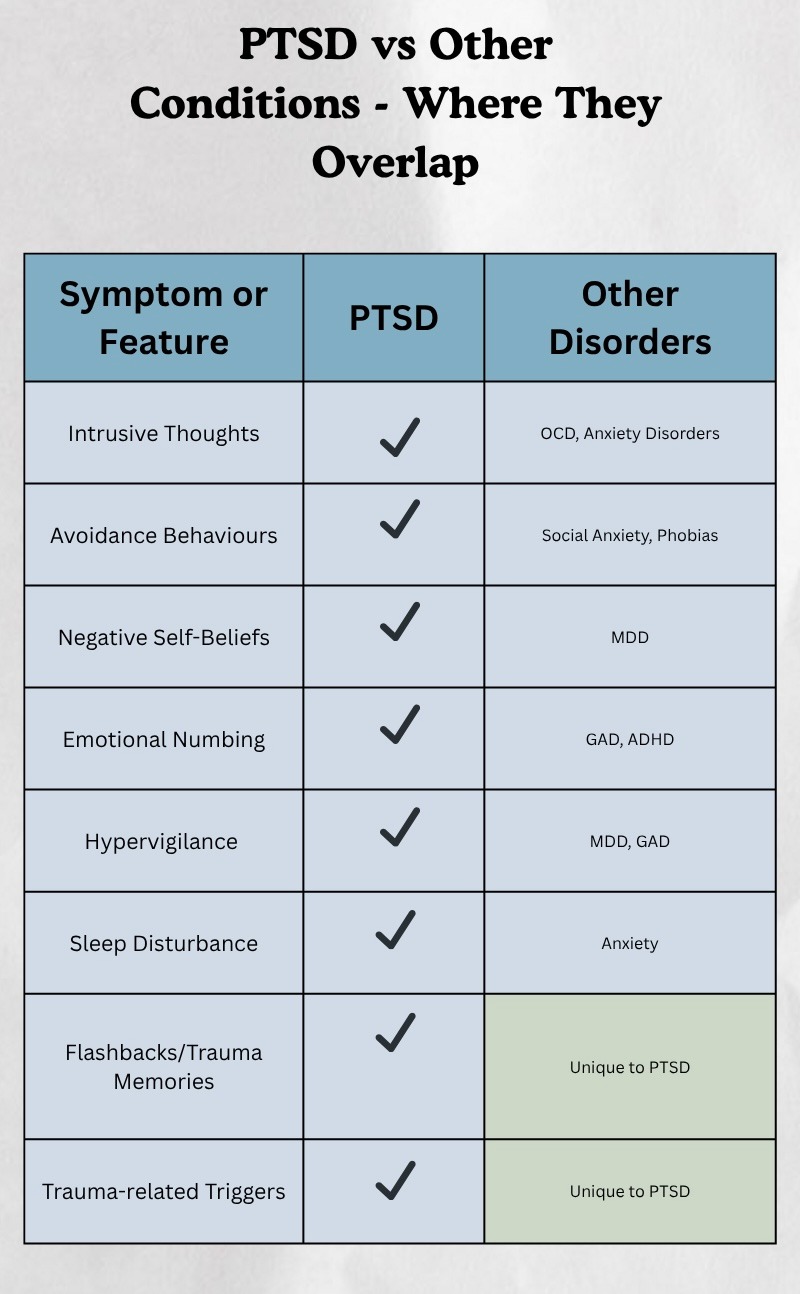
Symptoms associated with PTSD can overlap with anxiety, depression, OCD, or other concerns. Without a full clinical assessment, it’s easy to misinterpret what’s happening internally.
Impact on People Living With PTSD
Using terms like “trauma” or “PTSD” casually can unintentionally blur their meaning. For people living with PTSD, these experiences can be deeply disruptive and life‑altering. More precise language helps honour the weight of those realities.
Limiting Your Own Healing
When we label every painful experience as “trauma,” we may lose the nuance that helps us understand what we’re actually feeling. More specific language can open the door to deeper insight.
For example:
- “My breakup was traumatic.”
vs. - “My breakup was really painful. It made me question my self‑worth, and I’ve had trouble trusting people since.”
The second statement offers clarity, context, and direction for healing. It helps us understand what needs attention rather than collapsing everything into one word.
Why Nuanced Language Matters

Using more specific language doesn’t minimize our pain—it honours it. Naming our emotions and experiences with clarity can help us understand how they’ve shaped us and what kind of support we might need. It also helps us stay grounded in compassion for ourselves and others.
The goal isn’t to avoid the word “trauma,” but to use it thoughtfully and in ways that support growth, connection, and understanding.
Widening the Window: Tools for Regulation
If you notice yourself drifting toward the edges of your window, you can use "bottom-up" (body-based) strategies to help your nervous system settle back into the Optimal Zone.
If you are feeling Hyper-aroused (Too High):
The goal is to soothe and slow down.
- The 5-4-3-2-1 Technique: Name 5 things you see, 4 things you can touch, 3 things you hear, 2 things you can smell, and 1 thing you can taste. This pulls your brain out of "threat-mode" and back into the physical room.
- Long Exhales: Breathe in for a count of 4, and breathe out slowly for a count of 8. A long exhale signals to your Vagus nerve that it is safe to down-shift.
- Weight & Pressure: Place a heavy blanket on your lap or push your hands firmly against a wall. The resistance helps ground your energy.
If you are feeling Hypo-aroused (Too Low):
The goal is to gently wake up and reconnect.
- Sensory Input: Splash cold water on your face or hold an ice cube. The temperature change can "snap" the nervous system out of a freeze state.
- Movement: Gently stomp your feet or shake out your arms. This encourages blood flow and physical presence.
- External Focus: Pick a color and count every object of that color you can see in the room. This helps bring you back from a "spaced out" or dissociated feeling.
Conclusion
So, are we “traumatized”—or are we hurting in ways that deserve a different kind of language, care, and curiosity? When we move beyond labels and into nuance, we create space for deeper healing. Precise language helps us understand our experiences more fully and respond to them with compassion.
Ready to Move Beyond the Labels?If you’re navigating the impact of trauma or feeling stuck in cycles of stress, you don’t have to figure it out alone. At Vistas Psychotherapy & Wellness, our team of Registered Psychotherapists provides compassionate, evidence-based trauma support in Toronto, Ottawa, and across Ontario. We specialize in helping you understand your nervous system and find a path toward lasting healing. Book a Free 15-Minute Consultation
Let’s be gentle with ourselves and with each other as we navigate these conversations. Growth often begins not with a diagnosis, but with honest reflection and supportive dialogue. This post is for general educational purposes only. It is not therapy, does not replace individualized mental‑health care, and does not establish a therapeutic relationship. These reflections are offered to support understanding and conversation, not to provide diagnosis or clinical guidance. Other clinicians may hold different perspectives, and that diversity strengthens our community. If you’re experiencing distress or need support, please reach out to a qualified mental‑health professional in your area. If you are in immediate distress or at risk of harm, in Canada you can call or text 9‑8‑8 (Suicide Crisis Helpline) or call 9‑1‑1, and internationally you can visit FindAHelpline.com for free, confidential support.
Written by a student contributor and reviewed by a Registered Psychotherapist.
Citations
- Gardenswartz, C. (2024, July 26). Recognizing the impact of big T and little T trauma. Psychology Today. https://www.psychologytoday.com/ca/blog/the-discomfort-zone/202407/recognizing-the-impact-of-big-t-and-little-t-trauma?utm_source=
- McVay, E. (2023, August 31). Social media and self-diagnosis. Johns Hopkins Medicine. https://www.hopkinsmedicine.org/news/articles/2023/08/social-media-and-self-diagnosis
- Warner, D. (2025, September 6). Risk of mental health self-diagnosis: Chateau Health. Chateau Health & Wellness. https://www.chateaurecovery.com/the-potential-harms-of-mental-health-self-diagnosis-risks-and-realities
- Van, D. K. B. (2014). The body keeps the score : Brain, mind, and body in the healing of trauma. PenguinPublishing Group.

.jpeg)